Participation
BETs are time-consuming to compile, requiring systematic searching and reading of the literature, and detailed appraisal of evidence.
Each topic is written by one author, and reviewed by a second, for quality control purposes.
We have already completed a significant number of BET reviews, and begun the process of writing a great many more. However, we are keen to involve as many people as possible in writing BETs, to enable them to become a truly comprehensive knowledge resource.
If you would be interested in writing a BET, please use the submission form to register your intent. We recommend that you read several BETs, and the background documents on the site, to enable your BET to conform to the standard format. In particular, it is important that you submit a topic title and a derived three-part question of the form used in all BETs. If you have any queries about the submission process, please feel free to contact us. Completed BETs can be submitted using our online wizard.
We anticipate that a community may develop around this site, and we look forward to sharing ideas, experience and best evidence with colleagues from around the world.
How to do a BET
A working guide on how to plan, write and publish your BET review
- Professor Simon Carley
- Principal Lecturer and Honorary Consultant in Emergency Medicine
- Katharine Wylie
- Information Officer
On behalf of the BestBETs working group.
Contents
- Background
- Formulating your Question
- Searching the literature
- Appraising the literature
- How do you decide which papers to include in the table
- Relevance
- Quality
- The range of paper types
- Collating the data in the table
- Author, Date and Country
- Patient Group
- Study Type (level of evidence)
- Outcomes
- Key results
- Study Weaknesses
- Comments and the bottom line
- Getting published
- And finally
Background
The BETs system was set up at Manchester Royal Infirmary in 1996. As detailed in our original publications(1-3) they grew out of the single paper "Critically Appraised Topics" or CATs into a comprehensive strategy to detail the relevant evidence to precise clinical questions.
As with all systems we have adjusted and developed our techniques over the years in line with developments in the fields of evidence based medicine and information technology. The BETs have been fantastically successful with over 800 registered questions and over 300 publications. We now attract interest from all over the world and provide assistance to a wide variety of clinicians on developing their BETs.
The objective of this article is to describe how you get from your clinical question to your published BET.
What is a BET? (and what is it not!)
BET stands for Best Evidence Topic. We originally designed BETs as a systematic approach to answering real world clinical problems. It is an effective set of techniques to allow working clinicians to answer the important questions in their own clinical practice. We have evolved our methods over the years to identify a standard set of techniques to find clinical answers to clinical problems.
BETs use a systematic approach that is reproducible and explicit. By using a common format for publication BETs authors and the BestBETs team have answered hundreds of real world clinical problems. The standard format for reporting has allowed the development of a repository on the web and in the paper publication of BETs in a number of international journals.
BETs are not narrative reviews. We do not arbitrarily select papers that support a particular viewpoint, nor do we pick and choose which papers to use in order to support our personal views. The BETs author, using the BETs system can and should present all the evidence found in such a way that the reader can understand why the author came to the conclusion they did.
BETs are designed for the working clinician and therefore do not normally search the "grey literature" as is the case in formal systematic reviews. Whilst it would be an ideal for every clinical problem to be answered by a wide ranging systematic review and meta-analysis (if appropriate), this is not, and probably never will be the case. We at BestBets have much experience in the design and development of a number of systematic reviews and are fully aware of the amount of time these take (on average 6 months per question for one of our research fellows). As researchers we do not have the time to do systematic reviews in everything ourselves, and as clinicians we cannot wait for them to be completed in the future as our clinical problems exist today. BETs offer the reader and researcher a pragmatic systematic review for clinical practice. Where systematic reviews do exist we can incorporate these into the BETs model.
Where to start
Most BETs start when you are interacting with a patient and stop to think; why am I doing this? We encourage all members of our clinical team to constantly reflect on their practice, and critique their management of patients. If you think hard enough then there will be something about any patient that you see that makes you stop and consider what you are about to do next. Most of the time you just carry on and do what you have always done, but for the BET author it is time to see if that initial curiosity can be turned into an answerable question.
In this article we will refer to a hypothetical patient, Mr Jones, who fell whilst running, inverted his ankle and presented to the emergency department with a painful ankle. X-rays demonstrated an undisplaced fracture of the lateral malleolus distal to the joint line (a Weber A fracture).
Formulating your Question
Asking the right question
The BETs system works best when you can identify a specific problem and phrase it in such a way to allow it be answered. If you are doing a BET and get this bit wrong you can waste a hell of a lot of time. In our journal club we encourage new authors to bring their three part questions along even before they start searching so that they get it right at the beginning. It is terribly frustrating when people come along with a purportedly finished BET only to find out that it was critically flawed right at the outset.
We use the well known "three part question" system, which, unsurprisingly has three parts:
- Patient group
- Intervention or defining question
- Relevant outcomes
These three elements combine to form the question which then, and this is why it is so important, go on to define the search strategy that you will use to retrieve the evidence.
The patient group
Defining the patient group is essential and often takes a fair bit of thought. Making this completely specific to a small group (e.g. 35 year old men called Simon living in Gatley) means that if you find evidence it will be very applicable, but it does mean that you probably won't find any papers at all. One way to get this right is to write down your patient group in such a way so that someone working in the same field as yourself would be able to instantly imagine that type of patient in front of them. Try not to include terms that are irrelevant. A common error is to specify a particular sex or narrow age range when it is unlikely to make any difference to the eventual outcome.
Some examples:
- Good: Adults with undisplaced Weber A ankle fractures to the lateral malleolus
- Not so good: Patients with ankle fractures (too broad)
- Worse: Inuit men aged 18-28 with a Jones fracture to the 5th metatarsal following a fall from a horse (too narrow)
Intervention or defining question
Having decided which group of patients we are talking about we then need to think about what we are going to do to them. This will vary slightly depending on whether we are considering therapeutic questions, diagnostic questions, prognosis questions etc. but the basic design will remain the same. In therapy, diagnosis or intervention questions we typically compare one strategy against another, for example in a trial of a drug we may compare treatment A against treatment B or in diagnostics we may compare a gold standard against a new imaging modality or blood test. In prognostic studies we can usually define a factor that we suspect the outcome that affects the patient group.
What is essential, is that this section of the three part question defines what we think is influencing the outcome that we will define in the final part of the question.
For example, in our previous case of the patient with an ankle fracture a number of interventions could be considered.
- Are NSAIDs better than paracetamol at...
- Is tubigrip better than plaster of paris at...
- Is early mobilisation better than standard 4 week immobilisation at...
- Is MR scan better than X-ray for...
- Is physiotherapy better than simple advice at...
- Are active sportspeople more likely than sedentary people to...
Outcomes
Oddly enough this is the element of the three part question that often causes the most problems. If we are to practice in an evidence based way then it is vital that we are able to define what is an important clinical outcome. We see many questions that define an outcome as something rather vague like "making it better". It's difficult to measure "better" and it does not help with the searching.
Outcomes for the three part question should ideally be:
- Clinically relevant
- Patient orientated
- Definable
- Measurable
In many cases there will be more than one relevant outcome, that's fine, put them all down. You may not always find the evidence for every outcome but it is important to define what you and your patient think are important. Going back to our previous example we could define many different outcomes depending on which aspect of care was needed. Pain, disability (short and long term), return to work are all potential important outcomes for Mr Jones. An example of a complete three part question that might answer a clinical conundrum for Mr Jones doctor could be.
[In adult patients with an undisplaced Weber A fracture of the ankle] is [Tubigrip better than immobilisation in plaster of paris] at [decreasing pain, decreasing time to return of normal activities and/or improving eventual range of movement]
By convention we place square brackets around each part of the question, this helps us get everything in the right place.
If you have got this far, that's great. We would suggest that you now show your question to a colleague and ask them if it makes sense to them. Ideally show it to someone who has written their own three part questions in the past.
Once you have done this you are ready to register your question on the BestBETs website. This will allow the question to be registered under your name for a period of 6 months. You should also search on the database using the search function to make sure that no-one else has registered the question already. We will have a brief look at the question at this time and give feedback if possible. If you have not progressed with the question after 6 months we will contact you to see if you still want to keep it. If not, we will offer it to other BET authors as an available BET.
Searching the literature
Getting your search together
We suggest that you search using a variety of clinical databases. As a minimum we search Medline from 1966 to the present day. We also advocate searching in other databases such as Embase and on the Cochrane databases. Cochrane is always worth a look if you are considering a question related to therapy as you may find useful information in the form of a review or in their database of clinical trials (CENTRAL). If you do find a review that's fine, you can include it in your BET (once you have critically appraised it), but check the date of the review. If a systematic review has been done we usually include it in the BET, but also search in the other databases in the months and years following the last search published in the review. It is surprising how often you will find additional papers if you do this. As BETs was originally designed for the practicing emergency physician most searches on the database consist of Medline searches due to its accessibility.
How you actually input the search will depend upon which database you are searching and on also on which interface you are using. Despite this a few general principles will always apply. If you want help or advice with searching then you could speak to an experienced colleague, a librarian (or information scientists as we like to call them!) or have a look at some of the web sites on our links pages. Best of all you might like to consider coming on one of the BestBETs courses were we spend quite a bit of time giving you "top tips" and help on getting the best from your searching including a hands-on searching session.
Breadth of search
You should construct your search in such a way that it will have the best chance of finding any relevant papers. Remember we aim to define what evidence is available, not just cherry pick a few (superficially) high quality papers. So far, the majority of BETs have solely used Medline. Medline is good but we would also suggest that you should have a look at other databases, particularly the Cochrane database as this may turn up some additional useful information. For some questions, for example those related to nursing, you will need to use specific databases such as CINAHL which have a better coverage in these clinical topic areas. For advice on this we suggest you speak to your local medical librarian. There are no absolute restrictions on where you go looking for information to include in the BET. As long as it is explicit and that we can understand, follow and if necessary repeat it, it can be included in your search strategy.
We usually achieve this by using the three part question as a model. We start by looking at each component of the three part question and thinking of all possible terms relating to that element of the question. Most search engines have a thesaurus function that will assist you by interpreting any terms and suggesting index terms on the database.
The following examples and advice can only act as a short guide to our philosophy around searching. Different questions and databases will require different techniques. Unless you are an experienced searcher you will require help in ensuring that you have not missed any relevant papers. You may find help from some of the on-line guides to searching, from your local librarian or from the BestBETs course.
Try these:
One problem with many 3 part questions is that the outcomes section of the three part question often difficult to define in Medline terms (or any of the other databases for that matter). Consequently we usually combine all the terms from the patient group, together with all the terms referring to each component of the second part of the 3-part question. For example in a therapeutic question comparing treatment A with treatment B the search could be constructed like this:
[All terms to do with the patient group] AND [All terms to do with treatment A] AND [All terms to do with treatment B]
Or graphically:
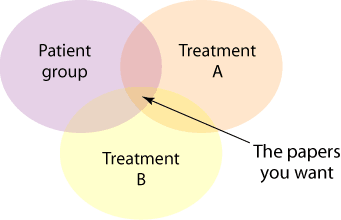
By putting all the terms together using an "OR" function you should be able to link in any relevant papers for each parts of the question. You can then combine each group together using an "AND" function to identify papers specific to the three part question.
The number of papers you get back will vary depending upon the search strategy and also on the topic itself.
If you get no papers or very few of poor quality:
- Have you put in all the relevant terms (e.g. generic and brand names of drugs)
- Check the thesaurus to make sure you have the right terms for that database (Remember that MeSH in Medline may not map to the same MeSH in Embase or CINAHL etc)
- Try a different database
- Broaden the terms relating to the patient group (e.g. instead of specifying a small age range, try all ages, the papers you find may still be relevant).
- Check your three part question
You may get an unmanageable number of papers from your search. When we started BestBETs we considered more than 50 unmanageable(3). However, with increased accessibility and internet speeds we will now look through up to 200 paper titles (sometimes more). If you still need to cut down the search then consider the following:
- If your search program has a LIMIT function then consider limiting your search to papers in languages you can read (though we recommend you at least look at the abstracts of these papers as the abstracts are often in English and you do not want to miss an important publication). In addition, excluding papers without abstracts will differentiate true papers from letters to journals (for example, by using the Boolean 'NOT' to exclude letters or editorials).
- You can look at your search terms again and consider making one aspect of it more specific (usually the patient group)
- If you are considering some technologies or conditions that did not exist before a certain date then limit your search to specific years.
- You may also use a "filter" to look for papers of certain types. Filters are a sequence of search terms that we use to identify papers of certain types, for example you may use a filter that will pick out any paper that is likely to be a randomised controlled trial. That would be particularly helpful if you were searching on a question comparing two different treatments. There are also filters in development for other types of papers but also for certain patient groups such as children, or for certain therapies such as steroids or antibiotics. For more information on searching in BestBETs and the use of filters please take a look at our search strategies information page. We also discuss filters on the BestBETs courses.
At this stage we suggest you write down your search strategy. This should detail:
- Which databases you searched
- What dates were searched (including both the start date and end date)
- Which interface (e.g. Ovid, PubMed, Dialog, etc) you used
- Which terms you used in each database
- If you found papers by some other means (e.g. in the references of another paper)
For example:
Search strategy
Medline 1966-09/04 using the Ovid interface and The Cochrane Library, Issue 3, 2004-10-01
Medline: [detail search terms here]
Cochrane: [detail search terms here]
Search Outcome
Altogether ** papers were found in Medline and ** in Cochrane, of which ** were irrelevant or of insufficient quality. A further ** papers were found by scanning the references of relevant papers. All relevant papers are summarised in the table.
Basically, anyone reading your BET should be able to repeat the search and understand completely how you came to the number of papers found that you state.
[To check whether people can follow the search, write it out and then re-input the search as it stands. If you arrive at the same number of papers then the search is correct and explicit!]
We consider up to 200 papers to be a manageable number to take onto the next stage.
The role of the second checker
All BET search strategies have at least two names attributed to them. The main author is the one who does most of the work! The role of the second checker is to ensure that the methodology is right.
The principle author should give the 3 part question ONLY to the second checker. It is then the role of the second checker to formulate their own search strategy and to try and find any relevant papers. They then take the second search strategy back to the principal author and compare the approaches. If the second search produces more relevant papers it should be adopted as the strategy for that BET.
The search checker should NOT just input the search terms used by the original author as that runs the risk of replicating any mistakes/omissions already made.
The search checker is also an ideal person to help construct the BET table. Show your BET table to them and see if it makes sense. If not rewrite it so that it does!
Appraising the literature
How do you decide which papers to include in the table?
Your search has probably given you a long list of papers that may or may not be relevant to your three part question. You need to decide which papers you are going to include in the eventual BET. We choose which papers to include using the following criteria.
- Relevance to the three part question
- The quality of the papers
- The range of different paper types
Relevance
It is usually possible to decide if a paper is relevant to the 3-part question by examining the title and abstract of the paper. This will tell you which papers you then need to get hold of and critically appraise. You can be quite ruthless at this stage by concentrating hard on which papers have the potential to answer your 3-part question. Remember, you are not attempting a wide ranging review of a broad subject, you are asking a specific, and focused question.
Quality
Once you have found your potentially relevant papers (the numbers should be well down by now) you need to get hold of them and critically appraise them. Getting hold of your papers can be difficult and you may need to get help from your local librarian. You do need to get hold of the full papers though. You simply cannot assess the quality of a paper from the abstracts you may have found on your search.
There are systems described that can help grade papers according to the way in which the trial is conducted. An example is the grading system shown below designed by Bob Phillips et al at the Centre for Evidence Based Medicine that relates the research methodology against the type of question being asked. Such an approach has merit but cannot be used in isolation. Even studies that may appear to be of a high level must still be individually critically appraised
Oxford Centre for Evidence-based Medicine Levels of Evidence (May 2001 published with permission):
| Level of evidence | Therapy / Prevention, Aetiology / Harm | Prognosis | Diagnosis | Differential diagnosis / symptom prevalence study | Economic and decision analyses |
|---|---|---|---|---|---|
| 1a | SR (with homogeneity*) of RCTs | SR (with homogeneity*) of inception cohort studies; CDR† validated in different populations | SR (with homogeneity*) of Level 1 diagnostic studies; CDR† with 1b studies from different clinical centres | SR (with homogeneity*) of prospective cohort studies | SR (with homogeneity*) of Level 1 economic studies |
| 1b | Individual RCT (with narrow Confidence Interval‡) | Individual inception cohort study with >80% follow-up; CDR† validated in a single population | Validating** cohort study with good††† reference standards; or CDR† tested within one clinical centre | Prospective cohort study with good follow-up**** | Analysis based on clinically sensible costs or alternatives; systematic review(s) of the evidence; and including multi-way sensitivity analyses |
| 1c | All or none§ | All or none case-series | Absolute SpPins and SnNouts†† | All or none case-series | Absolute better-value or worse-value analyses †††† |
| 2a | SR (with homogeneity*) of cohort studies | SR (with homogeneity*) of either retrospective cohort studies or untreated control groups in RCTs | SR (with homogeneity*) of Level >2 diagnostic studies | SR (with homogeneity*) of 2b and better studies | SR (with homogeneity*) of Level >2 economic studies |
| 2b | Individual cohort study (including low quality RCT; e.g., <80% follow-up) | Retrospective cohort study or follow-up of untreated control patients in an RCT; Derivation of CDR† or validated on split-sample§§§ only | Exploratory** cohort study with good††† reference standards; CDR† after derivation, or validated only on split-sample§§§ or databases | Retrospective cohort study, or poor follow-up | Analysis based on clinically sensible costs or alternatives; limited review(s) of the evidence, or single studies; and including multi-way sensitivity analyses |
| 2c | "Outcomes" Research; Ecological studies | "Outcomes" Research | Ecological studies | Audit or outcomes research | |
| 3a | SR (with homogeneity*) of case-control studies | SR (with homogeneity*) of 3b and better studies | SR (with homogeneity*) of 3b and better studies | SR (with homogeneity*) of 3b and better studies | |
| 3b | Individual Case-Control Study | Non-consecutive study; or without consistently applied reference standards | Non-consecutive cohort study, or very limited population | Analysis based on limited alternatives or costs, poor quality estimates of data, but including sensitivity analyses incorporating clinically sensible variations. | |
| 4 | Case-series (and poor quality cohort and case-control studies§§) | Case-series (and poor quality prognostic cohort studies***) | Case-control study, poor or non-independent reference standard | Case-series or superseded reference standards | Analysis with no sensitivity analysis |
| 5 | Expert opinion without explicit critical appraisal, or based on physiology, bench research or "first principles" | Expert opinion without explicit critical appraisal, or based on physiology, bench research or "first principles" | Expert opinion without explicit critical appraisal, or based on physiology, bench research or "first principles" | Expert opinion without explicit critical appraisal, or based on physiology, bench research or "first principles" | Expert opinion without explicit critical appraisal, or based on economic theory or "first principles" |
Produced by Bob Phillips, Chris Ball, Dave Sackett, Doug Badenoch, Sharon Straus, Brian Haynes, Martin Dawes since November 1998.
There are many publications on critical appraisal techniques for a wide variety of papers. All have their merits, pros and cons. We strongly advocate the use of critical appraisal checklists and have collated a number of these on the BestBETs web site where you can upload your critical appraisal on-line (these can subsequently be linked to the BET when you complete it). Many of the appraisal methods we use are based on the work of Crombie(4), Sackett (5;6) and Greenhalgh (7.)
Critical appraisal will allow you to decide if the conclusions of the study has any relevance to your question and also whether it has any validity. By assessing validity we are determining whether the quality of the study is sufficiently high to ensure that that the conclusions are justified. If during critical appraisal that the study is fatally flawed then make a note of this (and why) and discard it as it should not then be used in the BET. Ideally you will have done your critical appraisal on-line so that other readers can see why you discarded the paper.
Further guidance on the critical appraisal process is available on the BestBETs courses.
The range of paper types
For some topics all the papers you will find will be of similar design and quality. Often however, this will not be the case. As a general rule of thumb as to what to include in the BETs table we refer to the evidence levels shown above and take the papers from the highest level we found and those from the level below. For example you would take level 2 and level 3 papers if level 2 was the highest you found. If there is a high quality, relevant systematic review article (e.g. a Cochrane review) encompassing all relevant papers then include this and any subsequent relevant papers published after this date (i.e. there is no need to include each individual paper incorporated in the systematic review).
Collating the data in the table
If you go to the BestBETs database you will be able to see many examples of how other authors have summarised the data in the table. The basic table should look like this:
| Author, date and country | Patient group | Study type (level of evidence) | Outcomes | Key results | Study weaknesses |
|---|---|---|---|---|---|
Author, Date and Country
This should be fairly self-explanatory!
Patient Group
There should be enough information in this box so that the reader can understand who was studied and what happened to them. It often closely resembles the patient group/methods section of the abstract. However, it is important that you focus on elements related to the three part question. If you can make this brief that will help the editing process!
Study Type (level of evidence)
The basic study design is stated e.g. Prospective Randomised Controlled Trial, Diagnostic Cohort etc. If possible include the level of evidence from the CEBM table.
Outcomes
State in clear terms what the clinically relevant outcomes were for the paper in question. This should be unambiguous and directly related to the outcomes from the 3-part question. We discourage you from putting "interesting" data from the paper in this section. Remember that the BET is focused on answering your 3-part question and the outcomes should relate to this. By explicitly state we mean that the reader should be in no doubt what was measured. For example:
- Not so good: Movement improved
- Good: Time to return to normal sporting activities (in weeks)
- Better: Time to achieve full weight bearing
Key results
The key results and the outcomes sections of the table are directly linked. When the reader looks at the table they should see what was measured directly adjacent to the actual result in the key results section. You should put actual values in this column together with any measure of statistical analysis (e.g. a p value). It is not acceptable to just state that one thing is better than another. For good and bad examples see below:
| Outcomes | Key results |
|---|---|
| Time to return to full sporting activity | Mean of 35 days for tubigrip vs. 56 days for POP (t test p<0.001) |
| Able to fully weight bear | Mean of 14 days for tubigrip vs. 28 days for POP (t test p=0.05) |
| Self reported pain score at 1 week on 100mm VAS | 56mm for tubigrip vs. 60mm for POP (Mann-Whitney p=NS) |
| Range of movement | Better for POP |
[Note: I made all these figures up so don't quote me, it's just for illustration.]
As you can see the first 3 paired outcomes and key results allow you to interpret the findings in a meaningful way. The last pair lacks the detail required for the reader to know the magnitude or the significance of the effect.
Study Weaknesses
This is where you should put in details of any problems with the study. Generally these will consist of two elements.
Firstly, if there are methodological flaws in the study you should state them here. As we previously mentioned some studies will be so flawed that they were rejected at an earlier stage, they do not need to be included here.
Secondly, you should include comments here that relate to the applicability of the study data to your 3-part question. It is perhaps a little disingenuous to describe these as "study weaknesses" as it is unlikely that the authors had the BET in mind when they did the study. However, it is important for the reader of the BET to understand the applicability of the data to the question and the clinical scenario.
Comments and the bottom line
The comments section
This section is designed to allow you to further interpret the data and to discuss how you would use the evidence you have found to answer your clinical question. It may be that the evidence does not answer your question, fair enough, you should state this and if possible suggest why this is. Is it because the work has not been done, is of poor quality or that evidence exists but not specifically for your patient group (e.g. data only in adults for a paediatric question). The comments section is also an opportunity to bring in information that influences your real clinical decisions. For example, you may wish to comment on cost, training, resource issues. You may also wish to put the evidence within a wider framework of healthcare (for example how do specific injury patterns relate to child protection work).
Basically, the comments section is designed to put the evidence into context and to help the reader understand how you came to the clinical bottom line.
The clinical bottom line
OK, you have thought, questioned, searched, appraised, summarised and interpreted the data relating to your clinical question. It is time to get off the fence and decide what you are going to do. The clinical bottom line should ideally be a one sentence statement that directly answers your 3-part question. In fact you should be able to put the three part question next to the bottom line and it should make sense. If they seem unrelated then something has gone horribly wrong.
If you have not found the evidence to answer your question then you should state this. We usually say something along the lines of "No published evidence was found to answer the 3-part question: Local/National advice should be followed". We think this is a fair summary as it states the facts. It is also really useful information for clinicians. It is arguably as important to know where evidence is absent as to know about the published evidence.
Some BETs readers have found the negative BET (where no evidence is found) to be an irritation or at worst a waste of time. It is our belief that view is mistaken and that they are a valuable addition to the knowledge database in identifying areas for research.
Getting published
BETs are published both electronically and in paper form.
Electronic publication
You have by now almost certainly had a look at the web-based database of BETs. This is a way in which you can publish your BET to a wide audience (10,000 different people visit the site every month) of interested clinicians around the world.
Hopefully, you will have registered your question on the web-site after you finalised the format of your 3-part question. At that stage the question is reviewed by a member of the BestBETs team and put on the web site with a red colour code.
Once you have completed your BET you can then go back onto the web site and add all the additional information that you have collated. There is a rather nifty web based submission tool that takes you through each section of the BET. You don't even need to retype it all as you can cut and paste from Word into the web browser. Once you have uploaded all the data it is again read by a member of the BestBETs team to make sure that it is not libellous and posted on the site with a blue colour code signifying that it is complete but unchecked.
Blue BETs may be assigned a web editor who will then look at it in more detail and ensure that it meets the standard that we expect from our BET authors. When the web editor has reviewed the BET they may contact you to clarify any questions and to let you know of any changes we have made to ensure that it conforms with house style. Currently there is a backlog on these reviews so your BET may remain blue for some time.
Paper publication (by S. Carley)
BETs are now published (under various headings) in:
- Emergency Medicine Journal
- Archives of Diseases in Childhood
- Interactive Cardiovascular and Thoracic Surgery
- Emergency Nurse (soon!)
There are editors on all these journals who can select, commission and approve BETs that go forward to paper publication. There are no hard and fast rules about which BETs get selected though there are some that are more likely to get selected than others. It is my perception (SC) that those selected usually have the one or more of the following features:
- A high quality BET (good search, well constructed table, logical arguments etc)
- It addresses a common clinical problem
- It addresses a controversial topic
- It is a surprise (the evidence is contrary to common practice)
- It fits in with a theme issue of the journal
- The search has already been checked and re-run by a second author
At the moment I (SC) am not a member of any journal editorial boards so I can only give my impression from involvement in the project from the beginning (in other words don't quote me on this section!!!!).
BETs that are selected are re-searched and re-reviewed by senior members of the BestBETs team and the journal editors. If approved they are then changed to a yellow status indicating that it is an electronic pre-print. Finally, when published in paper format they are upgraded to Green.
Keeping the BET up to date
In the near future we will be updating the searches of all BETs on a 6 month rolling cycle. This will allow us to keep them up to date and to ensure that new evidence is added as it is published. If you write a BET and we do find new papers we will write to you and invite you to update it. We sincerely hope that you will be able to help maintain the database in as current a state as possible. Although not currently formalised many BETs have been and are regularly updated, you can identify recent changes with a specific icon on the database page.
And finally...
We hope this guide has been helpful. Let us know if any aspects of it are unclear or if there is anything else you would like to know and we will try and keep it up to date.
You can contact us at admin@bestbets.org or via the website.
Reference List
- Mackway-Jones K, Carley S. bestbets.org: odds on favourite for evidence in emergency medicine reaches the world wide web. Journal of Accident & Emergency Medicine 2000; 17(4):235-236.
- Carley SD, Mackway-Jones K, Jones A, Morton RJ, Dollery W, Maurice S et al. Moving towards evidence based emergency medicine: use of a structured critical appraisal journal club.[see comment]. Journal of Accident & Emergency Medicine 1998; 15(4):220-222.
- Mackway-Jones K, Carley SD, Morton RJ, Donnan S. The best evidence topic report: a modified CAT for summarising the available evidence in emergency medicine. Journal of Accident & Emergency Medicine 1998; 15(4):222-226.
- Crombie IK. The pocket guide to Critical Appraisal. London: BMJ Publishing, 1996.
- Sackett DL HRGGTP. Clinical Epidemiology: A basic science for clinical medicine. Boston: Little Brown, 1991.
- Sackett D. How to teach and practice evidence based medicine. 2nd ed. London: Churchill, 2000.
- Greenhalgh T. How to read a paper. The basics of Evidence Based Medicine. 2nd Ed ed. London: BMJ, 2001.
